THE human nervous system is composed of the brain, the spinal cord, and nerves branching off the spinal cord to the rest of the body. This system generates motion, regulates bodily functions, and transmits information about environmental conditions.
These functions are essential to life; hence the nervous system has several layers of protection: the brain is encased in the skull and suspended in cerebrospinal fluid; the spinal cord is encased in bone; individual neurons are insulated by a lipid-rich tissue known as the myelin sheath. Neurons rely on glia cells, which support neuronal homeostasis and are involved in myelination and remyelination.
Despite these natural defenses, the nervous system is susceptible to multiple degenerative diseases. Parkinson’s disease – marked by tremors, slow movements, and balance problems – develops when neurons die following a decrease in dopamine levels. Multiple sclerosis is a progressive loss of nerve function – symptoms may include weakness, tingling, and loss of motion control – caused by the immune system attacking the myelin sheath.
Alzheimer’s disease involves progressive neurodegeneration – or, damage to neurons and loss of communication between neurons – and, like many other conditions and diseases, is linked to aging, but its cause is currently unknown. Symptoms include loss of memory, difficulty thinking and making decisions, and behavioral changes.
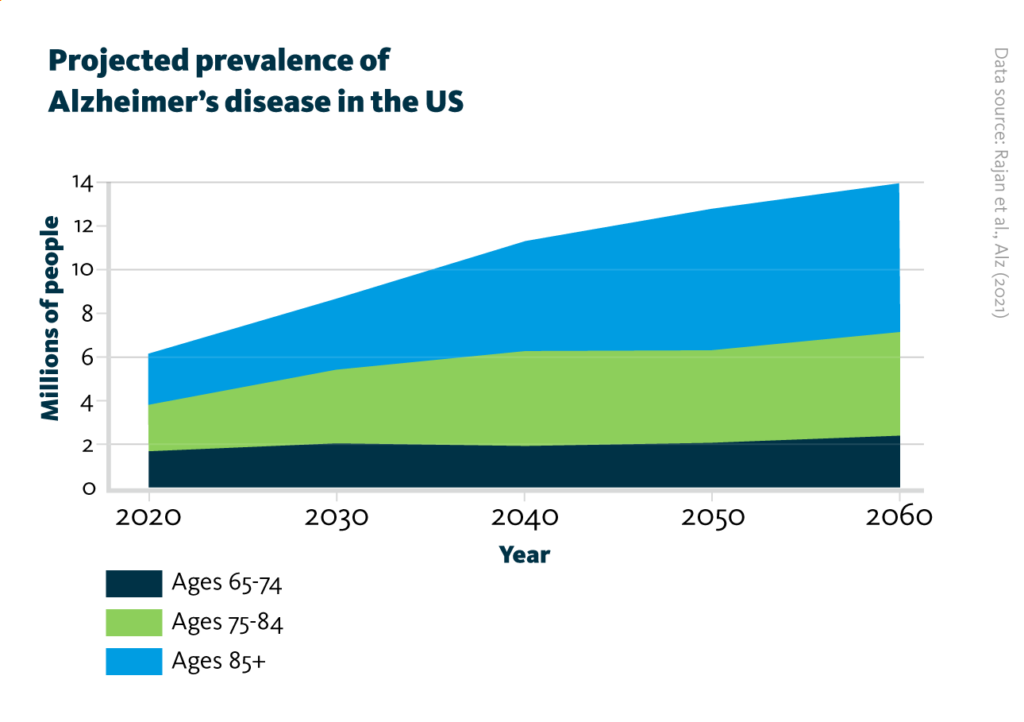
Projected prevalence of Alzheimer’s disease in the US: Projected number of people of age 65 and older (displayed as total and by age) in the US population with Alzheimer’s disease from 2020 to 2060.
Rajan et al., Alz (2021), doi: 10.1002/alz.12362
Currently, Alzheimer’s disease can be managed through pharmaceutical and behavioral interventions, but cannot be cured. For example, the tau protein aggregates into disruptive fibrils in the brains of Alzheimer’s disease patients; hence, it is a potent candidate for targeted drug delivery. A comprehensive understanding of the molecular and cellular signaling pathways involved in Alzheimer’s disease may inform the development of more accurate diagnostics and more effective therapies.
Multiomics technologies identify and quantity molecules – for example, proteins or lipids – in tissue samples. Through comparison of multiomics analyses across samples, molecular signaling pathways involved in physiological and pathological processes can be identified.
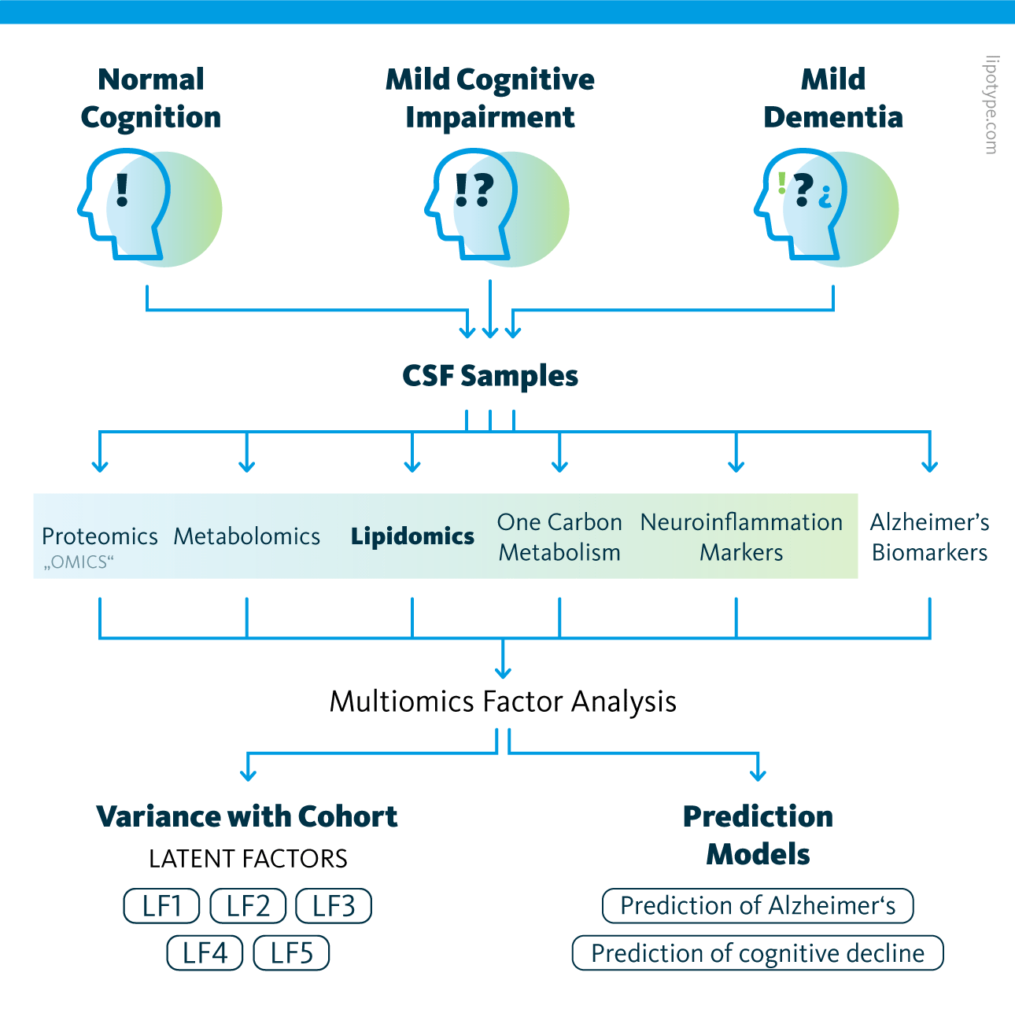
Study design schematic: Graphical outline of the multiomics cohort analysis of central nervous system pathway alterations in Alzheimer’s disease.
A research team from Nestlé Institute of Health Sciences combined multiomics technologies with statistical analyses to characterize molecular signaling pathways in cerebrospinal fluid to identify multiple molecules and signaling pathways associated with Alzheimer’s disease pathology.
The study cohort consisted of 120 people over age 55 evaluated at 0, 18, and 36 months. Participants were categorized into three groups – control, mild cognitive dysfunction, and Alzheimer’s disease – according to existing metrics for Alzheimer’s disease. These metrics are psychiatric examinations combined with ELISA assays on cerebrospinal fluid for expression of the proteins beta-amyloid 1-42 (Aβ1-42) and tau, and site-specific phosphorylation of tau (P-tau).
Cerebrospinal fluid samples were analyzed for known Alzheimer’s biomarkers and via multiomics: namely, proteomics, metabolomics, lipidomics, one-carbon metabolism, and neuroinflammation. The multiomics analyses identified 82 molecules that correlate with at least one of the known Alzheimer’s molecular disease biomarkers (Aβ1-42, tau, P-tau). The multiomics analyses also identified 37 metabolites, 29 proteins, and 5 lipids that correlate with the results of Alzheimer’s disease psychiatric examinations.
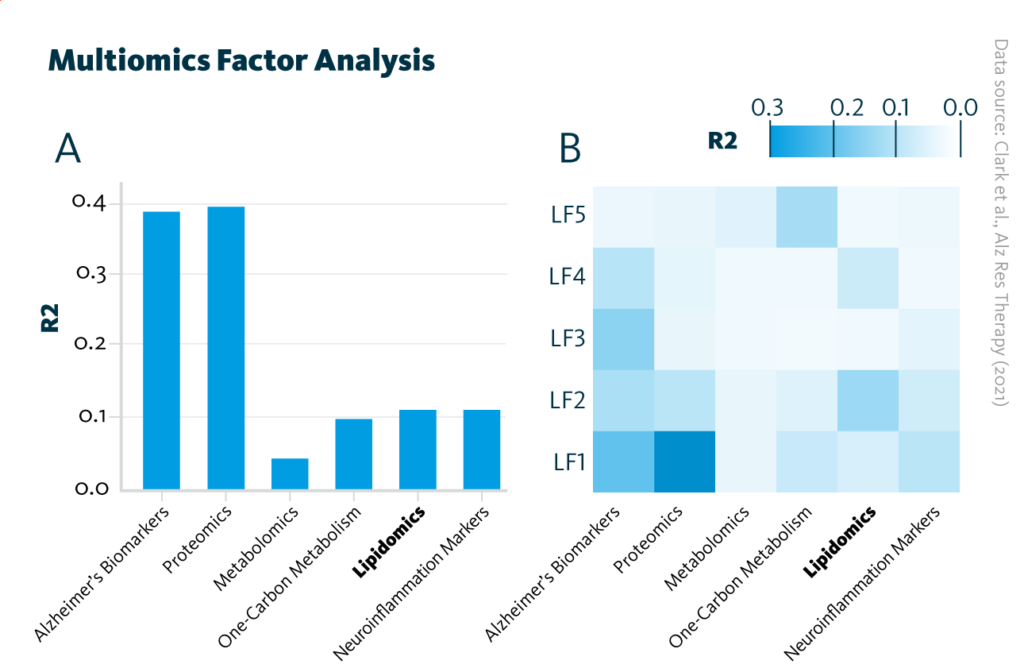
Multiomics Factor Analysis: Overview of the trained Multiomics Factor Analysis model showing variance (R2) within the cohort explained by A each analytical approach and B latent factors.
Clark et al., Alz Res Therapy (2021), doi: 10.1186/s13195-021-00814-7
To reduce the dimensionality of the multiomics data, a multiomics factor analysis was applied. The technique identified 5 latent factors that account for observed variance between participants. Each group of molecules – i.e., proteins, neuroinflammation markers, metabolites, or lipids – captures a portion of this variance.
While LF1 and LF2 were present in most multi-omics analyses, the remaining latent factors (LF3, LF4, and LF5) contributed comparatively little to overall variance and only captured variance across some multiomics data. Overall, Alzheimer’s disease biomarkers could explain for 38.5% of the variance; proteins accounted for 39.8%, lipids for 10.3%, neuroinflammation markers also for 10.3%, one-carbon metabolites for 9%, and other metabolites for 3.7% of the variance.
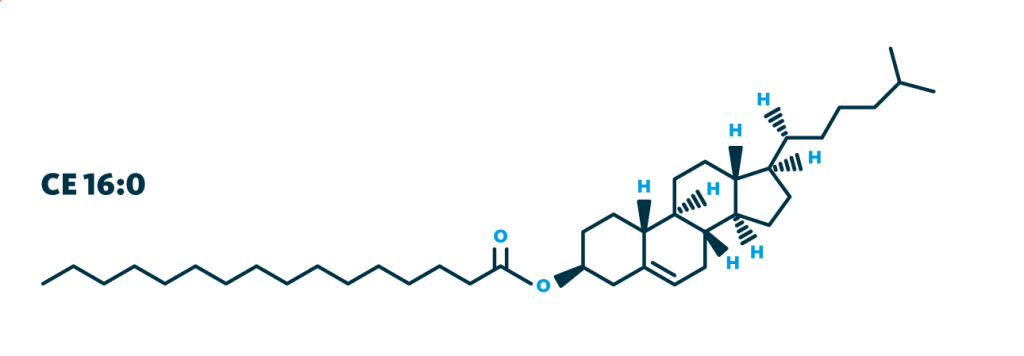
The cholesteryl ester associated with Alzheimer’s disease: Molecular structure of the lipid cholesteryl ester 16:0 that was linked to LF4, one of the five latent factors that account for the variance between Alzheimer’s patients which was observed through multiomics analysis.
Each of the five latent factors exhibits unique correlations with both the multiomics analytes and the existing Alzheimer’s disease biomarkers. This suggests that the latent factors may represent specific molecular pathways involved in Alzheimer’s disease. For example, the sterol lipid cholesteryl ester 16:0, which had not been linked to Alzheimer’s previously, correlates with latent factor 4.
Careful examination of these relationships suggests that latent factors 1-3 reflect neuronal injury, while latent factors 4 and 5 are indicative of amyloid pathology and aid in prediction of cognitive decline.
Next, two molecular signatures linked to Alzheimer’s or cognitive decline were derived from the multiomics factor analysis. Both contained four molecules each and improved the sensitivity and specificity of predictive models for cerebral Alzheimer’s disease and cognitive decline, respectively.
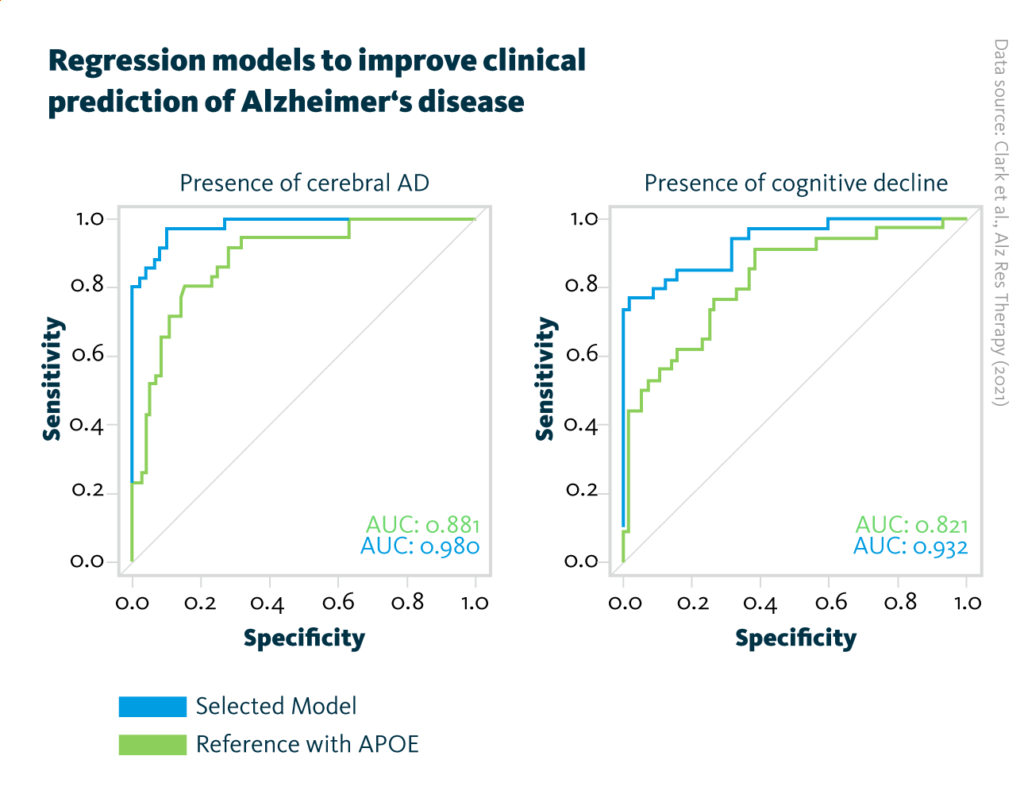
Regression models to improve clinical prediction of Alzheimer’s disease: AUC curves for the final prediction models obtained after addition of the four respective analytes selected by the MOFA model of Alzheimer’s pathology (blue, left graph) and cognitive decline (blue, right graph). For comparison, the reference model including APOE status information (green, both graphs) has been added.
Clark et al., Alz Res Therapy (2021), doi: 10.1186/s13195-021-00814-7
The 4-molecules combination that improved prediction of cognitive decline contained the lipid that was previously linked to latent factor 4: cholesteryl ester 16:0. This further hints at lipid pathway alterations without a direct link to core Alzheimer’s pathology but having impact on the rapidity of cognitive decline.
Overall, this study demonstrates that multiomics analyses of cerebrospinal fluid can identify cellular and molecular pathways involved in Alzheimer’s disease, which can improve predictive models of pathology.
Integrated multiomics analyses have identified molecular signaling pathways involved in Alzheimer’s disease, cardiovascular diseases, cancer, and type 1 diabetes. Through comprehensive characterization of pathology, these multiomics analyses may identify novel therapeutic targets and/or diagnostic biomarkers.




Lipotype Lipidomics characterizes the lipid composition in patient samples. When combined with proteomics, metabolomics, and other multiomics technologies, these data may identify molecular signaling pathways involved in both physiological and pathological processes such as Alzheimer’s disease.
Do our methods apply to your samples?
Let’s figure that out!

Lipotype products are provided for Research Use Only. They are not intended for clinical diagnostic purposes and must not be used to inform medical treatment decisions. The content of this article is for scientific and educational purposes only and should not be considered medical advice.