LIPID metabolism – the process through which the body synthesizes and degrades lipids and fatty acids for energy, signaling, structure, and other physiological functions – is regulated by circadian rhythms. Therefore, it is altered in people with atypical sleeping cycles, including those who work night shifts. Unfortunately, changes in lipid metabolism are also linked to metabolic diseases, including cancer and diabetes.
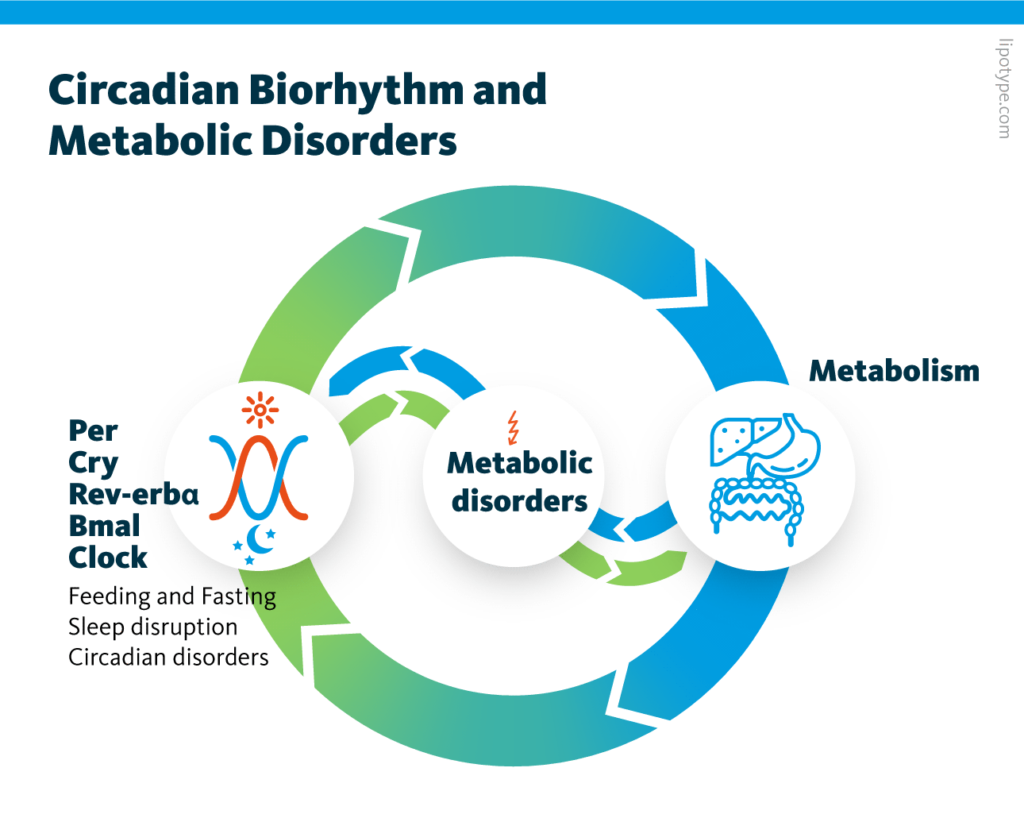
Diabetes is a set of metabolic disorders marked by a loss of glycemic control, that is, the ability to regulate glucose concentrations in the blood via insulin. Glycemic control can be partly monitored via insulin sensitivity, a measure of the body’s responsiveness to insulin. In type I diabetes, the pancreas stops producing insulin; this condition is called insulin deficiency. In type II diabetes, the tissues in the body stop responding to insulin; this condition is called insulin resistance.
Insulin sensitivity, which may be linked to lipid metabolism, is reduced in type II diabetes and thus may be an early indicator of disease onset. However, the molecular mechanisms that contribute to insulin sensitivity remain unclear, hindering both diagnostic and therapeutic efforts.
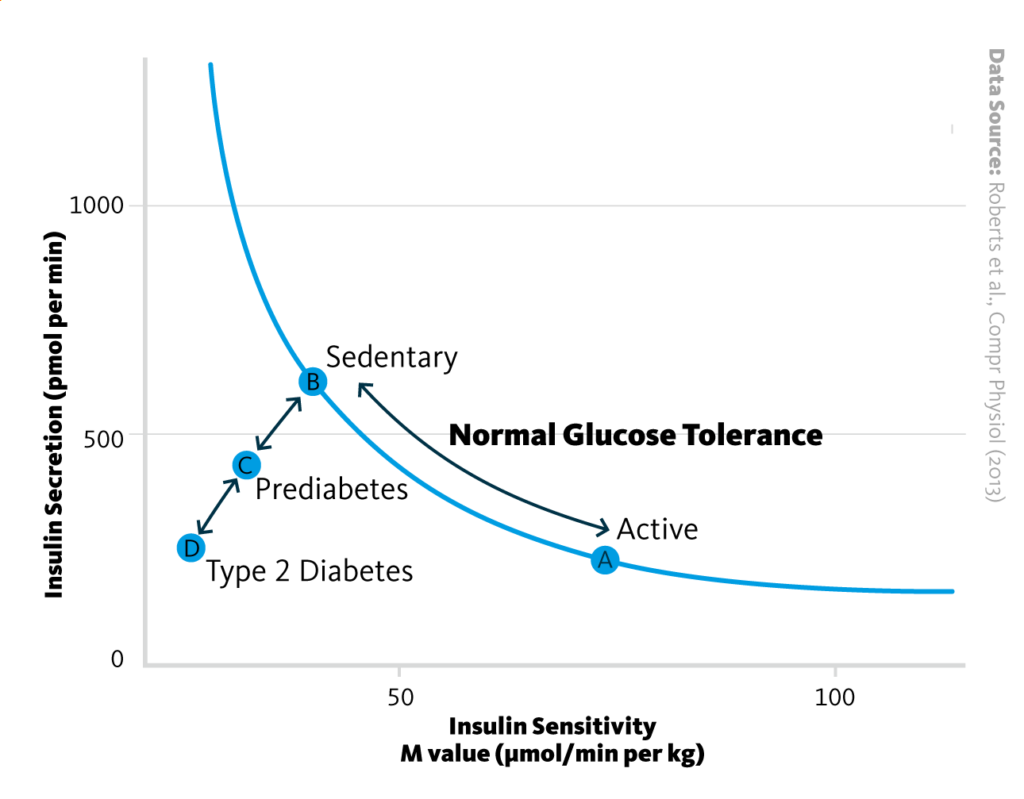
Insulin sensitivity and diabetes: Insulin sensitivity is reduced in type II diabetes, reduced insulin sensitivity is an indicator of prediabetes.
Roberts et al., Compr Physiol (2013), doi: 10.1002/cphy.c110062
Current research suggests that lipidomic analyses can classify lipid metabolism dysfunction – for example, metabolic obesity – more accurately than traditional metrics. This observation may enable researchers studying insulin sensitivity and diabetes prevalence to monitor population health more precisely.
Recently, a research team led by the German Institute of Human Nutrition and the German Center for Diabetes Research employed lipidomic analysis of blood plasma samples to examine how meal timing and composition affect lipid metabolism and glycemic control, with a focus on insulin sensitivity.
The study cohort included 29 non-diabetic men who consumed two iso-caloric test meals, one in the morning and a second in the afternoon. The two test meals were either high-carbohydrate or high-fat. This first intervention phase lasted two weeks. During the second two-weeks intervention phase, the order of the meals was reversed. A 4-weeks washout phase separated the two intervention phases from each other.
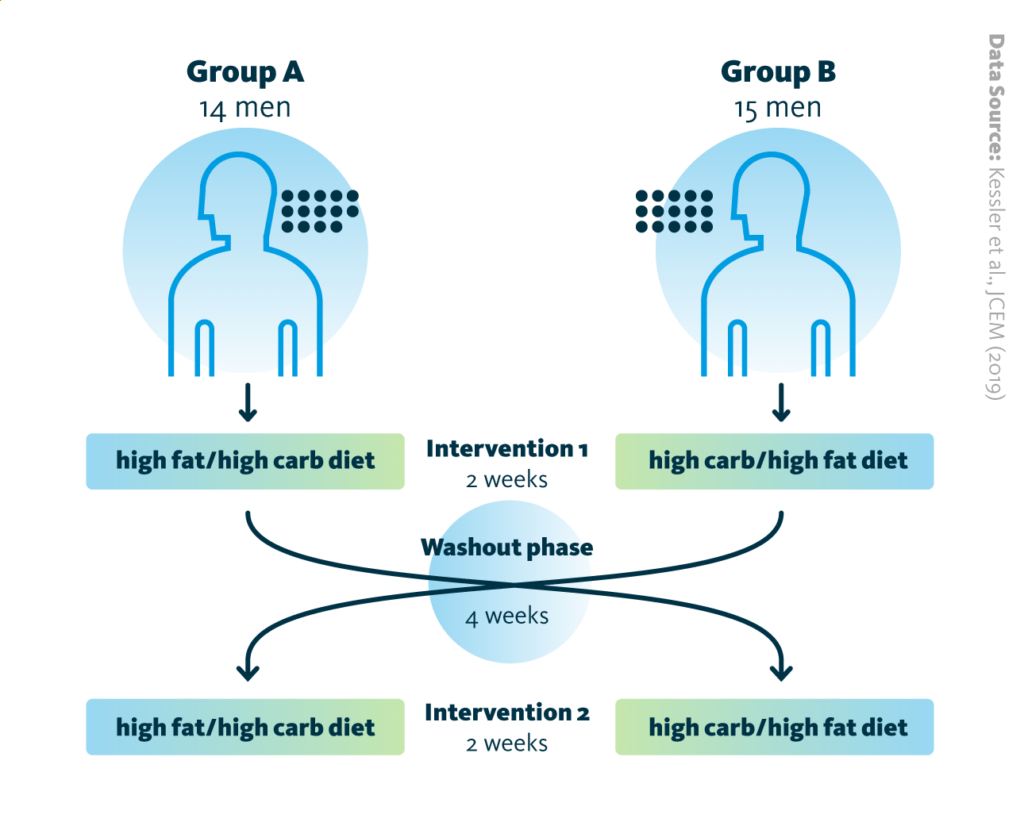
Study design schematic: Graphical outline of the intervention study to analyze the relationship between circadian lipid metabolism and insulin sensitivity.
Kessler et al., JCEM (2019), doi: 10.1210/clinem/gdz176
To monitor lipid metabolism and glycemic control, blood and subcutaneous adipose tissue samples were collected from participants before and after meal consumption and analyzed via lipidomics, biochemical assays, and qPCR. One-third of participants showed impaired insulin sensitivity.
Lipidomic analysis of the blood identified 672 different lipid species from 14 lipid classes, of which 233 appeared in at least 70% of all samples. Of the 233 lipids, 67.8% varied over the course of the day,1.3% were affected by the meal composition, and 55.4% exhibited dependence on both time and nutritional content. These findings indicate that lipid metabolism is regulated by meal timing and composition, which is consistent with earlier studies.
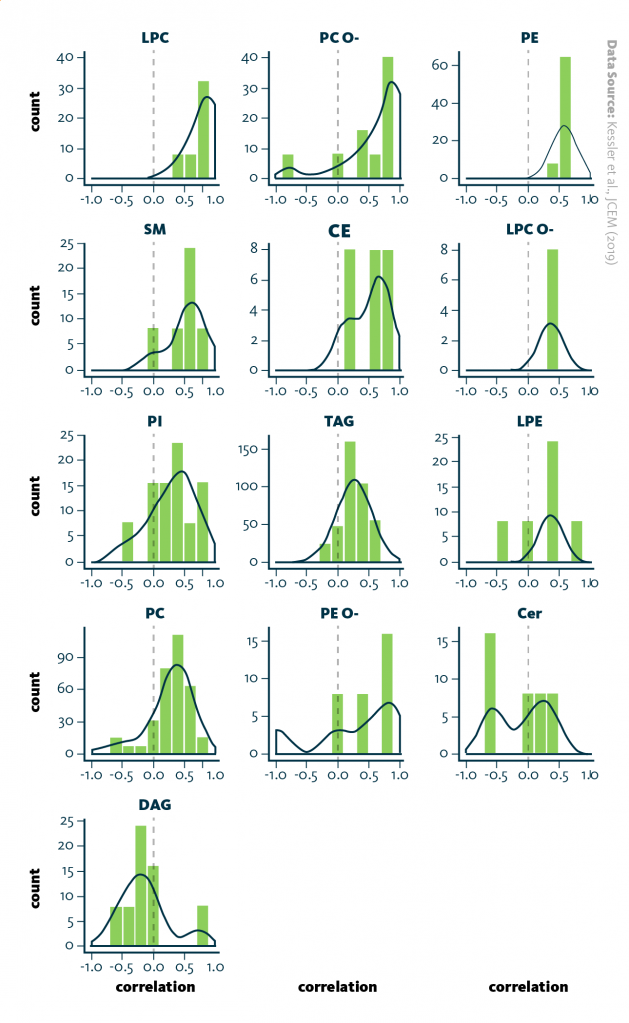
Comparison of daily lipid profiles: Correlation of daily lipid profiles across lipid classes. Lipid class enrichment is shown as histogram with overlayed density plot. The distance of the peak from the dotted line (correlation coefficient r=0.0) indicates how similar (r>0.0) or different (r<0.0) the daily lipid profiles in each lipid class are between the two diets. Only lipid species with high coherence within the cohort (diff>1.5) were included in the analysis.
Kessler et al., JCEM (2019), doi: 10.1210/clinem/gdz176
To probe the relationship between lipid metabolism and time more closely, the study examined the plasma lipid profile after a morning versus afternoon meal. Following a high-carbohydrate meal, the concentrations of ester phospholipids, namely phosphatidylethanolamine and lyso-phosphatidylethanolamine, and glycerolipids were higher after a morning versus afternoon meal. Following a high-fat meal, the concentrations of the same lipid classes plus cholesterol were elevated in the morning compared to the afternoon.
For both high-carbohydrate and high-fat meals, the lipid profile following morning meals was enriched for triglycerides with short fatty acid chains, further supporting the finding that lipid metabolism depends on the time of day. Additionally, insulin secretion and sensitivity in the blood decreased in the afternoon, which was accompanied by a high concentration of glucose.
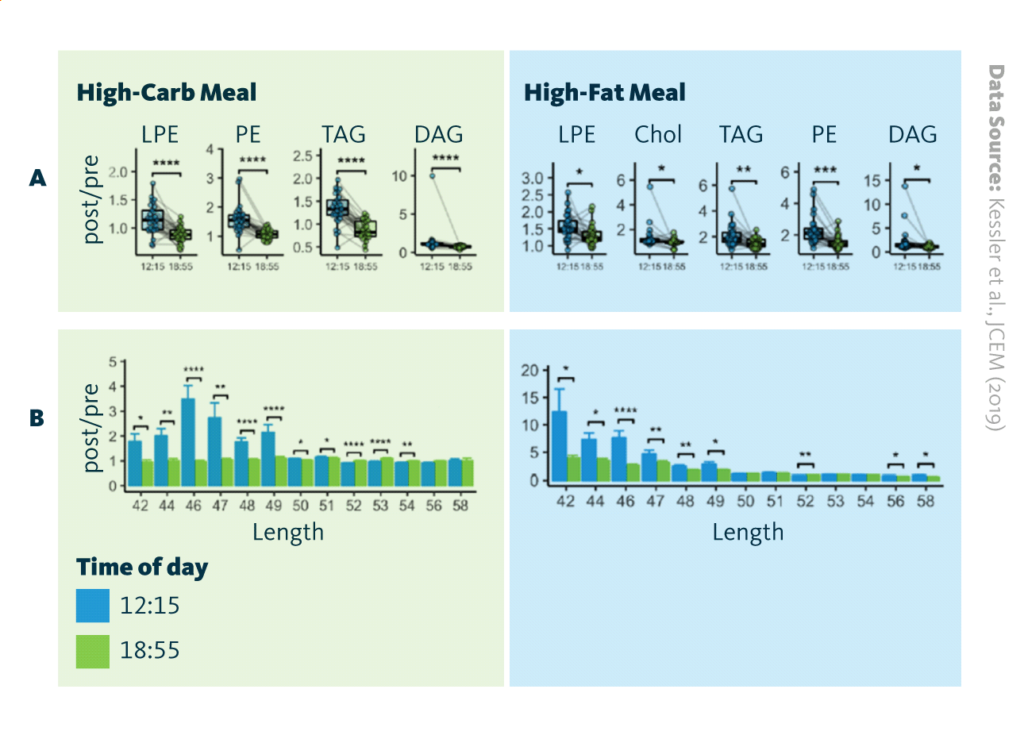
Postprandial lipid responses in the morning versus afternoon following a high-carbohydrate or high-fat meal: A Diurnal differences of lipid classes. Values for individual subjects are displayed as points and connected by lines, the overall shape of the distribution is shown as a boxplot. B Diurnal differences of triglyceride postprandial responses dependent on total triglyceride chain length.
Kessler et al., JCEM (2019), doi: 10.1210/clinem/gdz176
In search of a molecular mechanism to explain these temporal changes in lipid metabolism, the report characterized gene expression in adipose tissue. As expected, expression of genes known to regulate circadian rhythms varied with the time of day. Expression of enzymes involved in fatty acid synthesis and metabolism was higher following a high-carbohydrate versus high-fat meal but did not change with the time of day, which accounts for the plasma lipidome’s dependence on meal composition but not time.
Overall, this study characterizes how meal timing and composition impact the plasma lipidome. The results identify a relationship between lipid metabolism and insulin sensitivity. Additional studies will describe the molecular mechanisms driving these observations, including the involvement of circadian rhythms.




Lipotype Lipidomics technology can monitor changes in lipid profiles over time and in response to stimuli. These data may enable scientists to detect, predict, and characterize metabolic dysfunction and resolve outstanding questions about the relationship between lipid metabolism, insulin sensitivity, and circadian rhythms.
Do you have any questions?
We can answer them!

Lipotype products are provided for Research Use Only. They are not intended for clinical diagnostic purposes and must not be used to inform medical treatment decisions. The content of this article is for scientific and educational purposes only and should not be considered medical advice.